Umbilical Catheters
)
What is an umbilical catheter?
Umbilical catheterisation is a procedure performed by highly skilled neonatal clinicians shorty after birth in premature or critically unwell neonates1. The procedure allows for central venous and arterial access, enabling administration of medications and fluids, painless blood drawing, and continuous blood pressure monitoring2,3.
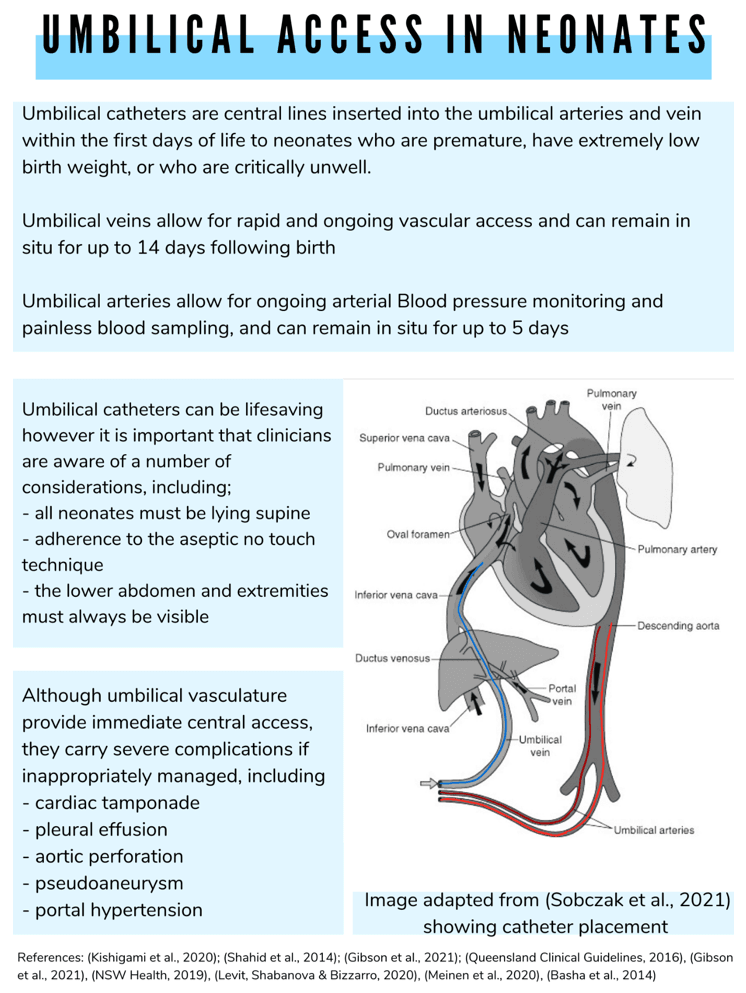
Umbilical venous catheters are inserted through the umbilical vein and travel through the ductus venosus, through to the inferior vena cava, right below the right atrium3. They are often inserted in a resuscitative situation following birth, where the neonate requires resuscitative fluids or adrenaline4. The line can remain in situ for up to 14 days and can be used for ongoing medication and fluid administration until decisions regarding further vascular access can be made3.
Umbilical arterial cathetersextend from the umbilical artery through the internal iliac artery and can be placed as high as above the diaphragm and just below the subclavian artery3. They should not be used for fluid or medication administration, and instead can be used for continuous blood pressure monitoring and blood sampling. Unlike venous catheters, arterial catheters can only remain in situ for five days3,5.
Management
Neonates must be placed supine with the lower abdomen and extremities exposed to enable frequent assessment of the site, and allow for earlier monitoring of the extremities to prevent serious complications as a result of a catheter being placed incorrectly, thus interrupting blood flow2,6. Aseptic non-touch technique is critical whenever manipulating the catheters and administration sets.
Complications
Complications largely arise from either a malpositioned catheter or infection7. Complications of malposition include cardiac tamponade, pleural effusion, hepatic portal hypertension, and aortic perforation, which can all have serious impacts on short and long-term health8. A major risk is catheter line-associated bloodstream infections (CLABSI)2. Neonates are at a significantly increased risk of serious complications as a result of infection, due both to an immature immune system and underlying maternal conditions in the antenatal period9.
References
1. Kishigami M, Shimokaze T, Enomoto M, Shibasaki J, Toyoshima K. Ultrasound-guided umbilical venous catheter insertion with alignment of the umbilical vein and ductus venosus. Journal of Ultrasound Medicine 2020;39(2):379-83.
2. Shahid S, Dutta S, Symington A, Shivanda S. Standardising umbilical catheter usage in preterm infants. Pediatrics 2014;133(6):1742-52.
3. Gibson K, Sharp R, Ullman A, Morris S, Kleidon T, Esterman A. Risk factors for umbilical vascular catheter-related adverse events: a scoping review. Australian Critical Care 2021.
4. Queensland Clinical Guidelines. Neonatal Resuscitation; 2016; Available from: https://www.health.qld.gov.au/__data/assets/pdf_file/0011/140600/g-resus.pdf.
5. Gibson K, Sharp R, Ullman A, Morris S, Kleidon T, A. E. Adverse events associated with umbilical catheters: a systematic review and meta-analysis. Journal of Perinatology 2021.
6. NSW Health. Umbilical Catheters: Care and Management in CICU. 2. Sydney Children’s Hospital Network; 2019; Available from: https://www.schn.health.nsw.gov.au/_policies/pdf/2016-1000.pdf.
7. Levit O, Shabanova V, Bizzarro M. Umbilical catheter-associated complications in a level IV neonatal intensive care unit. Journal of Perinatology 2020;40(4):573-80.
8. Meinen R, Bauer A, Devous K, Cowan E. Point-of-care ultrasound use in umbilical line placement: a review. Journal of Perinatology 2020;40(4):560-6.
9. Basha S, Surendran N, Pichichero M. Immune Responses in Neonates. Expert Review of Clinical Immunology 2014;10(9): 1171-1184. https://doi.org/10.1586/1744666X.2014.942288
| Tags:central vascular access devicesumbilical catheters |








