AVATAR Multimedia
Explore webinars, educational tools, research resources, and global training content to advance vascular access care and infection prevention.

Podcast: Dr Grace Xu on PIVCs in the Emergency Department
INS Infusion Room (Season 2, Episode 5) explores the hidden risks of routine IV insertion in the ED, with practical insights on improving insertion practice, evidence-based care, and patient-centred approaches for difficult venous access.
Listen to the Podcast
Webber Training Teleclass Education
Free global teleclasses on infection prevention, patient safety, and healthcare innovation. Access recordings, slides, and join a worldwide IPC network.
Read More
Evidence-Based List of Vesicant Medications
Presented by Lisa Gorski, Lynn Hadaway & Barb Nickel for AVATAR.
Watch Video
Wiser Wound Care
Update on Peripheral IV Catheter Clinical Care Standards. Learn how to prevent wound complications and improve outcomes.
Watch Now
Essential Practices for CVADs
Free and informative resources from Cancer Institute NSW & eviQ Education.
View ResourceCentral Venous Access Devices
Series of 8 videos on clinical procedures for central venous access devices by Cancer Institute NSW and eviQ Education.
Watch Videos
eviQ CVAD Course
Course to support and guide CVAD clinical management using best available evidence.
Start Course
Assessing a Peripheral IV Cannula
Ausmed video by Dr Gillian Ray-Barruel, Senior Research Fellow with AVATAR.
Shared with permission by Ausmed (www.ausmed.com.au)
Watch Video
miniMAGIC - IV Catheter Guide
Quick video by A/Prof Amanda Ullman + MAGIC guidelines for safer IV choices.
Dr. Vineet Chopra (U-M Medical School, VA Ann Arbor, and IHPI) introduces the Michigan Appropriateness Guideline for Intravenous Catheters (MAGIC), a research- and consensus-based tool to help choose the safest, most appropriate IV device for each patient.
For consumers: http://umhealth.me/PICCvid
For clinicians: http://umhealth.me/piccvid2
I-DECIDED® Assessment Tool
Evidence-based, valid and reliable vascular access device assessment and decision tool.
Watch Video
IV Flushing Video
Excellent teaching video: IV Maintenance - Application of Science to Practice.
Watch Video
Central Venous Catheter (IJV)
The emergency procedures team have taken a deep dive into artificial evidence tools and had a hard think about many of the details on this procedure.
Watch Video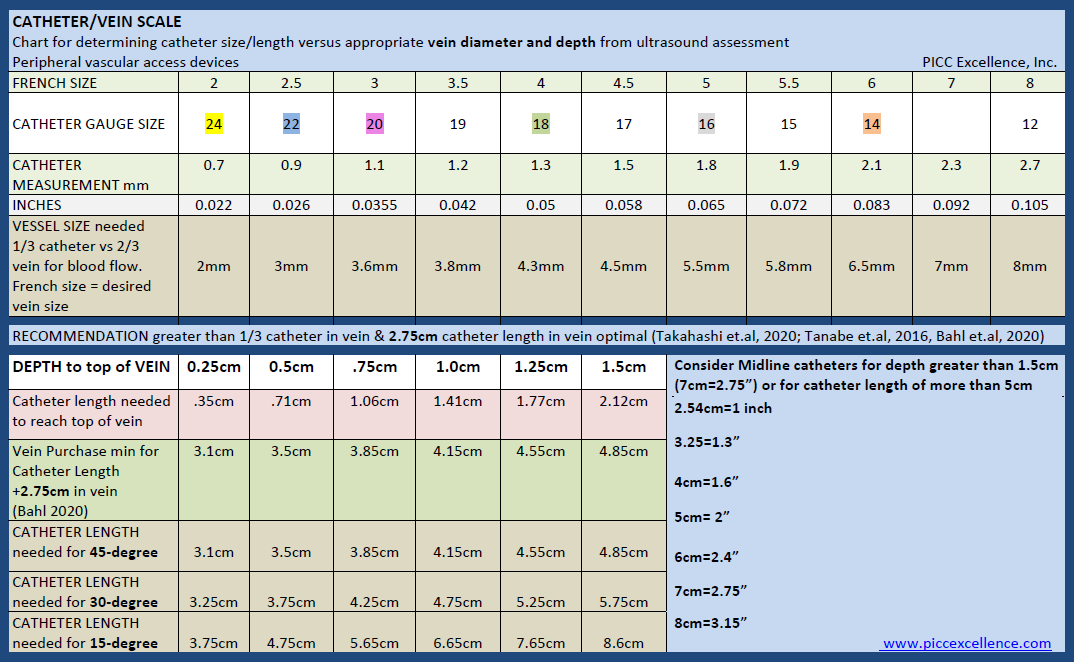
Catheter/Vein Scale
Chart for determining catheter size/length versus appropriate vein diameter and depth from ultrasound assessment.
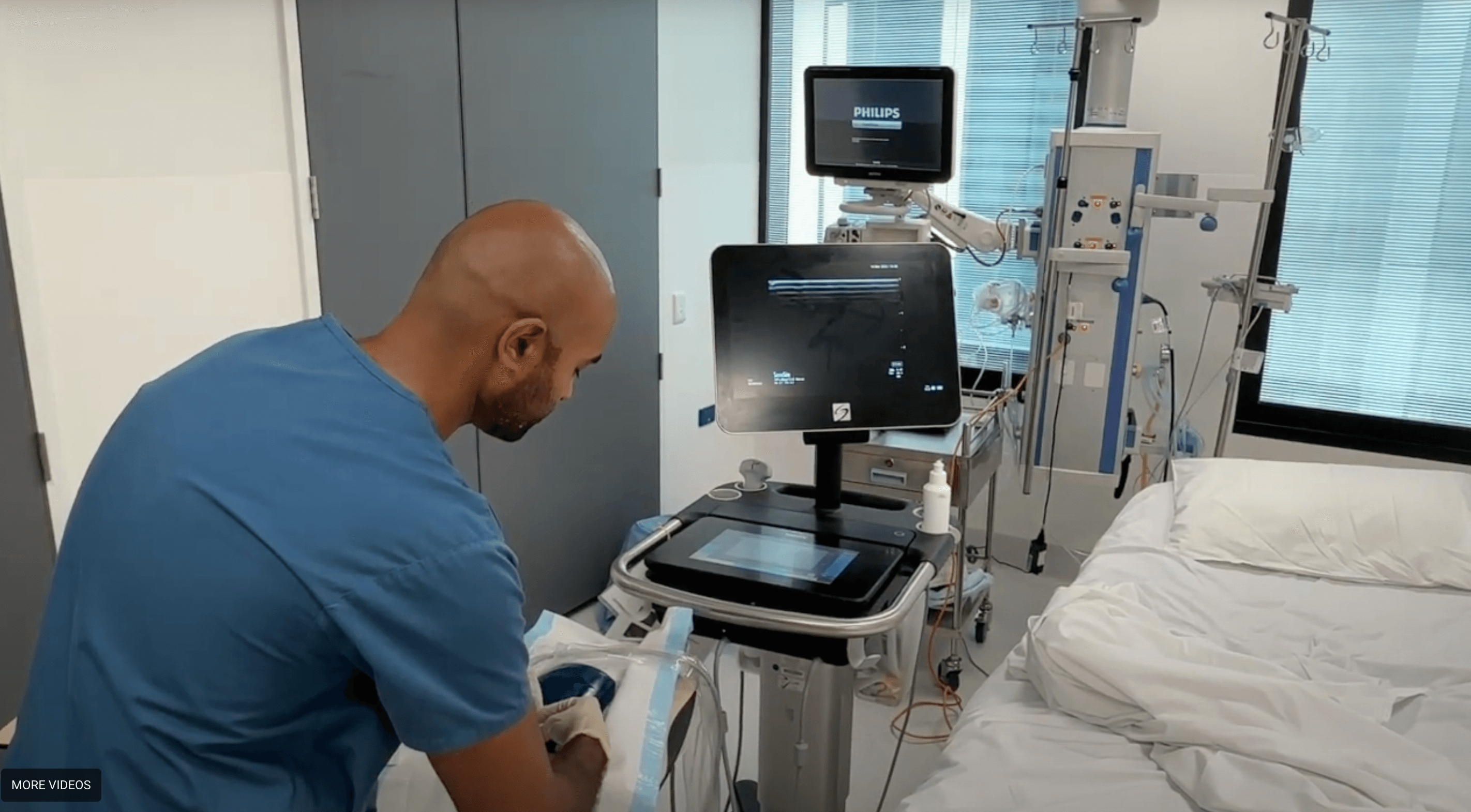
Ultrasound Guided Vascular Access
Overview of the process and procedure with top tips for success
Watch Video
Practice Guidelines for Central Venous Access 2020
An updated report by the American Society of Anesthesiologists Task Force on Central Venous Access.
Read Guidelines
DIVA Blood Collection Service
Mini documentary on ultrasound-guided pathology specimen collection, improving patient engagement and reducing painful attempts.
Watch Video
State of the Art in Vascular Access Seminar
Videos from the 2017 AVATAR seminar covering PIVCs, CVADs, and paediatric vascular access.

PIVC Insertion, Maintenance & Removal
AVATAR educational video, developed with Baxter, showing best practices to reduce complications and failures.
Watch Video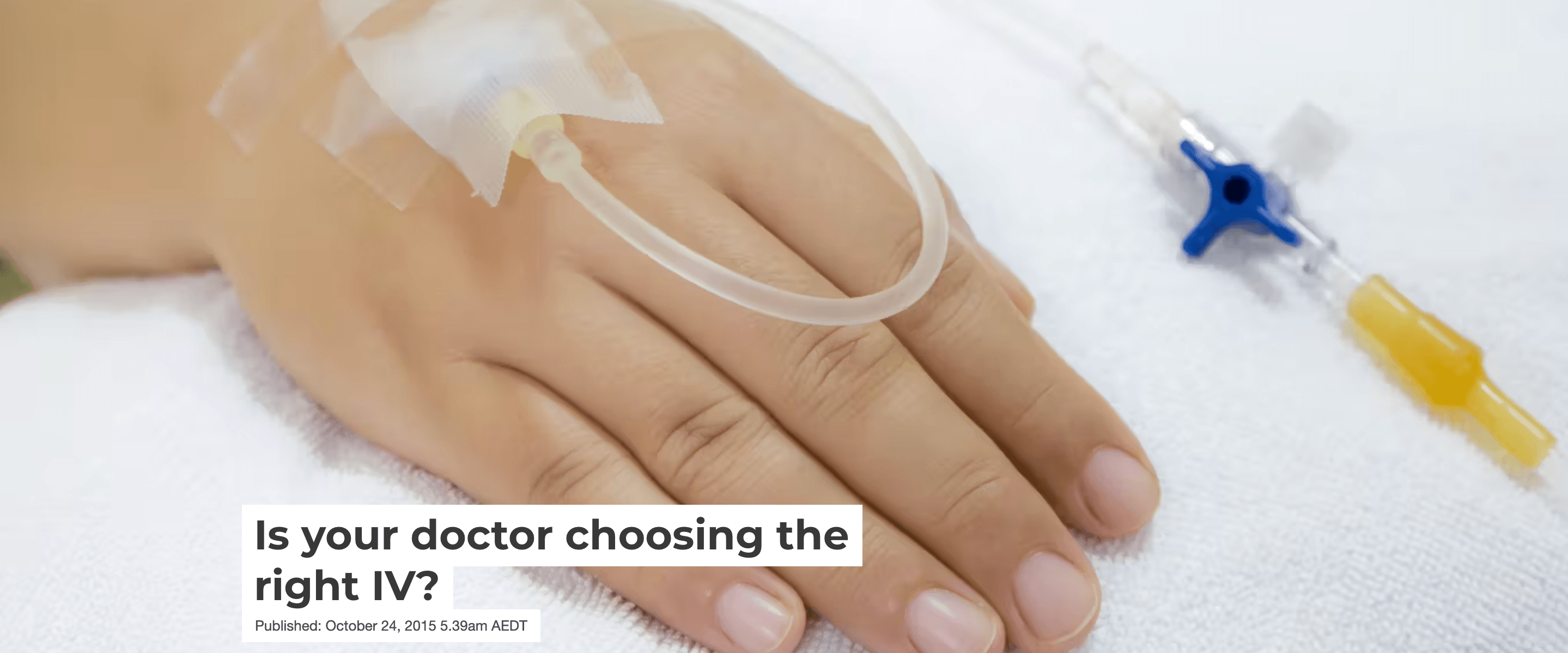
Is Your Doctor Choosing the Right IV?
Article in The Conversation by Dr Vineet Chopra & Dr Scott Flanders.
Read Article
IV Device Infection Risks Webinar
20-minute ACIPC webinar presented by Dr Gillian Ray-Barruel from AVATAR Group.
Watch Video
Clinically Indicated Site Rotation
Presentation by Marcia Wise at AVA ASM 2015 on moving toward clinically indicated site rotation.
Watch Video







