Posted in peripheral intravenous catheter
Taking Blood Samples from a PIVC: Yes or No?
Posted by Dr Linda Coventry
on 21 March 2023
We are often asked if it's okay to take blood samples from a peripheral intravenous catheter (aka PIVC, cannula). In Australia, each state has a different policy, however, most allow blood draws on insertion of the cannula.
The Infusion Nurses Society Standards of Practice 8th edition (2021, page S129) has the following recommendations, based on evidence:
"Risks associated with sampling from a PIVC include hemolysis of the sample, contamination of the sample from infusing...
| Posted in:peripheral intravenous catheterevidence-based practiceblood sampling |
INS Webinar: PIVC Bundles
Posted
on 24 June 2022
| Posted in:peripheral intravenous cathetereducationIV management |
CNSA Vascular Access Devices: Evidence Based Clinical Practice Guidelines: Online launch 3 November!
Posted by Kerrie Curtis
on 28 October 2021
)
Vascular access devices are lifelines for patients with cancer for the administration of prescribed therapies and supportive care. Evidence-based management is key in the prevention of vascular access complications and premature removal.
The revised Cancer Nurses Society of Australia (CNSA) Vascular Access Devices: Evidence Based Clinical Practice Guidelines detail the latest evidence and recommendations for patients with cancer with peripheral intravenous cannulas and central venous ac...
| Posted in:peripheral intravenous cathetercentral vascular access deviceseducationpatient safetyguidelinesevidence-based practice |
Aseptic non-touch technique (ANTT®)
Posted by Lizzy Ostwald
on 26 October 2021
)
Aseptic non-touch technique (ANTT®)
Aseptic non-touch technique (ANTT®), a framework developed by Rowley in the 1990's, focuses on the identification and prevention of microbial contamination of aseptic parts or sites during clinical procedures. ANTT® ensures aseptic parts or sites are not touched - either directly or indirectly, ensuring sterility during procedures that can cause significant patient harm if performed incorrectly1. Since its conception, ANTT® has bee...
| Posted in:peripheral intravenous cathetercentral vascular access devicesvascular access devices |
PIVCs in Neonates: Caution advised!
Posted by Lizzy Ostwald
on 20 September 2021
)
Peripheral intravenous cannulation (PIVC) is commonplace in the neonatal setting, particularly in premature and critically unwell neonates who are unable to regulate homeostatic balance.1
Cannulation of a neonate can be difficult, given the significantly smaller venous anatomy and compromised skin integrity which can lead to localised toxicity and inflammation.2 Failure rates can be high, with 95% of PIVCs being removed due to complications including occlusion, leaking and extravasation inju...
| Posted in:peripheral intravenous catheterassessmentneonate |
Tips for PIVC Location and Size
Posted by Lizzy Ostwald
on 19 August 2021
Of the 11 million Australians accessing care in a hospital each year, an estimated 7.7 million will receive a peripheral intravenous catheter (PIVC), also called a cannula, meaning this procedure is commonplace, particularly in the emergency department.(1) Although this is such a common procedure, first-attempt failure rates are high, with an estimated 40% failure rate in adults and 65% in the paediatric population.(1)
All clinicians who are cannulation competent must be abl...
| Posted in:peripheral intravenous cathetercannulapatient experienceIV insertionvessel health |
PIVCs in the Emergency Department
Posted by Lizzy Ostwald
on 15 July 2021
)
The emergency department is a fast-paced, hectic and often unpredictable environment. In the 2019-2020 financial year, Australian EDs treated 8,236,159 patients, reviewing an average of 22,600 patients per day (1). Often working under duress and having to make clinical decisions within a very narrow timeframe, ED clinicians must quickly identify what a critically unwell patient needs in order to be stabilised (2,3).
Achieving vascular access usually means urgent insertion of a peripheral ...
| Posted in:peripheral intravenous catheterinfection preventioninsertionvascular access devices |
Can I draw blood from a PIVC?
Posted by Lizzy Ostwald
on 7 July 2021
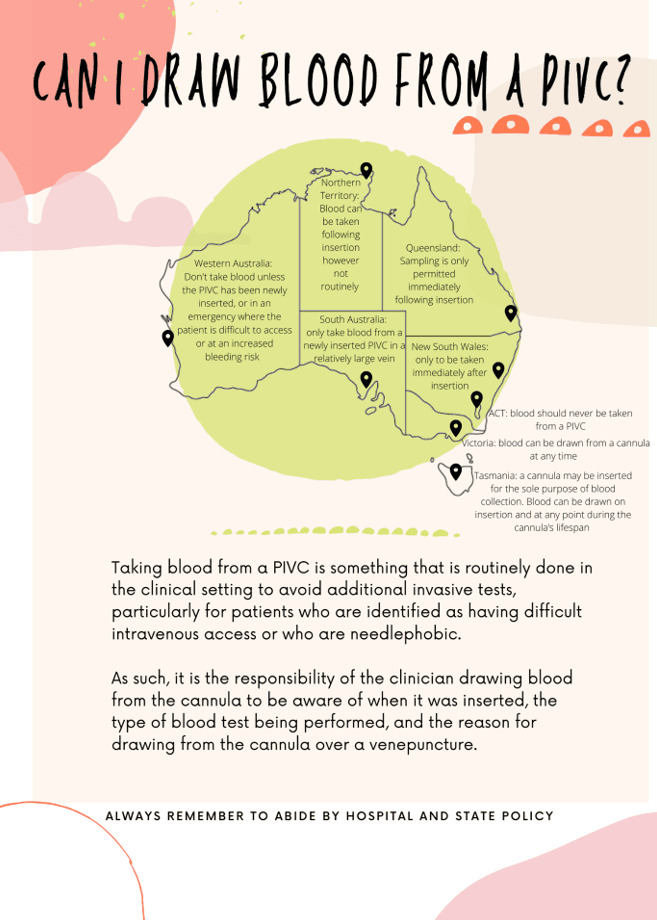)
Drawing blood from a cannula is a routine practice in some clinical environments. But is this best practice or will the blood become too haemolysed to provide accurate results?
Drawing blood from a peripheral intravenous catheter/cannula (PIVC) is a routine practice in clinical environments such as the emergency department, rationalised as one less invasive test that a patient is subjected to. A PIVC should never be inserted just to draw blood or 'just in case' it's needed late...
| Posted in:peripheral intravenous catheterblood samplingvenepuncture |
Preventing IV complications podcast
Posted by Gillian Ray-Barruel
on 5 July 2021
Those who know me understand how passionate I am about PIVC care!
In this Osler podcast, Dr Todd Fraser and I discuss best practice of PIVC insertion and maintenance, with essential tips for infection prevention and good cannula assessment and management.
If you like this podcast, I encourage you to check out the Osler website and download the free My Osler app. They have lots of excellent education podcasts and learning modules for all kinds of healthcare professionals. ...
| Posted in:peripheral intravenous catheterdressingseducationinfection preventionsecurement |
PIVC Essentials: Three Tips for New Grads
Posted by Lizzy Ostwald
on 28 June 2021
)
"Hi, I'm Lizzy, and I'm in my final semester of a dual bachelors of nursing and midwifery, and am fortunate to be undertaking a Winter Research program with the AVATAR group. I have decided to focus on tips for a new grad as my first topic as I am going to be a grad at the start of next year, and I believe that a lot of benefit can be gained from easy access to summarised, accurate information."
Coming into the hospital setting as a graduate nurse, or 'grad...
| Posted in:peripheral intravenous cathetercannulaIV managementevidence-based practice |









